Volume 1, Issue 1
Article Type: Research Article
The role of care unit coordinators and reference professionals in person-centered care for people living with dementia in nursing homes
Abel Catela-Huertas1; Sandra Pinzon-Pulido2*; Patricio J Fuentes-Maltes3; Cristina Fernandez-Portero4
1El Roble, SCA Sevilla, Spain.
2Andalusian School of Public Health, Granada, Spain.
3CG El Buen Samaritano - Caritas Diocesana, Málaga, Spain.
4Universidad Pablo de Olavide, Sevilla, Spain.
*Corresponding author: Sandra Pinzon-Pulido
Professor, Andalusian School of Public Health, Granada,
Spain.
Email ID: sandra.pinzon.easp@juntadeandalucia.es
Received: Feb 10, 2025
Accepted: Mar 04, 2025
Published Online: Mar 07, 2025
Journal: Annals of Pediatrics and Neonatal Care
Copyright: Pinzon-Pulido S et al. © All rights are reserved
Citation: Catela-Huertas A, Pinzon-Pulido S, Fuentes-Maltes PJ, Fernandez-Portero C. The role of care unit coordinators and reference professionals in person-centered care for people living with dementia in nursing homes. Ann Gerontol Geriatr Res. 2025; 1(1): 1001.
Abstract
The person-centered care approach has been demonstrated to have benefits for individuals with dementia residing in residential care facilities and the professionals who care for them. However, its implementation remains challenging, particularly because it necessitates a substantial shift in care culture. To facilitate its application in these settings, the roles of the living unit coordinator and reference professionals have been introduced. These professionals share the responsibility of getting to know the individuals they care for through their life history and organizing their care around their wishes and preferences. The core element of this approach is the establishment of meaningful connections and relationships between the individual receiving care and the caregiver. To support these changes, the living unit coordinator adopts a transformational leadership style, based on their ongoing presence in the unit, as well as their role in demonstrating, supervising, and guiding the transition in professional practices.
Keywords: Dementia; Nursing homes; Long-term care; Person-centered care; Unit coordinator; Reference professional.
Abbreviations: PCC: Person-Centered Care; NVivo: Qualitative data analysis software.
Introduction
Person-Centered Care (PCC) for Individuals with dementia has been shown to meet their essential needs for comfort, attachment, inclusion, occupation, and identity [1]. This approach is predicated on a culture of care that respects the autonomy of those receiving care and fosters the development of bonds between them. The environment must be designed to be homelike and comfortable, and to facilitate meaningful daily activities [2].
There is sufficient scientific evidence indicating the benefits of this approach in residential settings, both for the person receiving care and for the staff providing care. This approach fosters the stability necessary for the development of trusting relationships and for staff to become acquainted with the residents under their care [3,4].
Despite its merits, the implementation of this approach is confronted by numerous challenges, including staff attitudes and beliefs. Staff members may be accustomed to a conventional approach to care that is centered on tasks, rigid routines, and standardized procedures, making it difficult to adopt a more personalized and flexible approach that respects the preferences and wishes of each individual. Resistance to change, inadequate training, and high workloads can reinforce unresponsive attitudes toward a more humanized model. In addition, some professionals may not recognize the importance of involving residents in making decisions about their own care, perpetuating paternalistic dynamics [5,6].
To facilitate the implementation of this culture of care, the creation of two professional figures is recommended: the unit coordinator and the reference professional. In practice, the unit coordinator is entrusted with a limited number of assistants, responsible for the care and support of a small group. She is tasked with facilitating the adoption of new professional practices and adapting the environment to promote this change. The referral professional, in contrast, is an auxiliary who is assigned two or three people. This professional is responsible for inquiring about their life history and gathering their wishes and preferences regarding their care and daily life in the center. The referral assistant creates an emotional bond with each person and is the one who maintains direct contact with the family for day-to-day matters [7].
The following study explores the perceptions of professionals who have adopted these roles and the strategies they use to advance the implementation of the PCC approach in their centers.
Materials & methods
A qualitative study was carried out based on 11 in-depth interviews with 4 coordinators and 2 reference professionals from residential centers implementing the PCC approach in Andalusia (Spain). The interviewees were women, aged 39 to 64 years and had between 4 and 22 years of experience in their job.
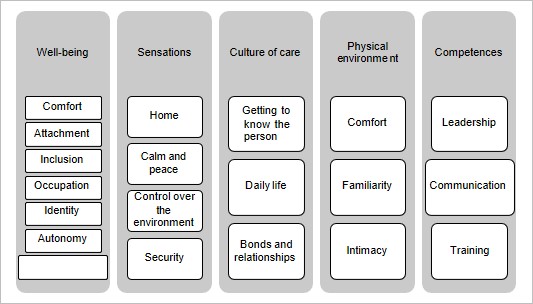
The interviews were recorded, transcribed and analyzed with the support of NVivo 11. The discourse analysis collected the emerging themes derived from the experiences and perceptions of the participants. These themes were grouped according to the key categories proposed by Catela et al. [2] to which were added leadership, communication and training (Figure 1).
Table 1: Main themes identified in the discourse of the unit coordinators interviewed.
| Competences | ||
|---|---|---|
| Leadership | Communication | Training |
| The unit coordinators highlight the importance of transformative leadership that allows them to change the daily practices of direct care staff. To achieve this, it is necessary to remain in the cohabitation unit for an extended period. Any modification in professional practice is implemented through a phased approach, commencing with the initial demonstration of the new method, followed by the provision of ongoing supervision and support until the revised practice becomes integrated into the unit's daily routine. | The unit coordinator must cultivate her active listening, empathy, and assertiveness skills. Communication is imperative not only with her team of assistants but also with individuals living with dementia and their families. The unit coordinator assumes the role of an ally and becomes an integral member of the professional team that provides care for the residents of the unit. | The unit coordinators' training, as well as that of their professional teams, is of particular importance. Training should encompass the person-centered care model, the management of behavioral symptoms of dementia, and the modification of professional practices. The most efficacious method to effect a change in professional practice is through face-to- face and practical training conducted on a day-to- day basis. |
| Culture of care | ||
| Getting to know the person | Daily life | Bonds and relationships |
| Unit coordinators emphasize the importance of becoming acquainted with each individual, understanding their life history, and observing them to identify their sources of satisfaction. The unit coordinator also assesses methods to maintain or improve the person's functional and cognitive abilities through activities that are meaningful to them. This knowledge of the person is shared with the team of assistants who care for them. | One of the most important changes in person- centered care is the relaxation of daily routines. The transition from a focus on tasks to a focus on people presents a significant challenge for the unit coordinator and their professional team. Unit coordinators also highlight the need to slow down, to be calmer when carrying out daily tasks, in order to adjust to the preferences and desires of people with dementia. | The fundamental principle of person-centered care is predicated on the establishment of bonds and meaningful relationships among the individuals constituting the living unit, including those with dementia, their families, relevant professionals, and unit coordinators. The development of such bonds and meaningful relationships is contingent upon the stability and availability of auxiliary staff, who must allocate sufficient time to establish a personal connection with each individual. |
| Well-being | ||
| Autonomy | Occupation | Identity |
| The primary challenge confronting unit coordinators is to guarantee that the team of care assistants facilitates the exercise of individuals with dementia's right to make decisions regarding their daily affairs and to manage decisions that entail risks for the individual. The ability to exercise autonomy necessitates a degree of flexibility in daily routines and an understanding of individuals' preferences and wishes. | A primary responsibility of a living unit is to implement activities that are meaningful to individuals with dementia. These activities should be aligned with the patients' life histories, preferences, and current desires. The unit coordinator assists the team of care assistants in identifying and organizing such activities, with the objective of engaging the patients and promoting their well-being. | The process of identifying individuals living with dementia necessitates comprehensive observation and a comprehensive understanding of their past and present life circumstances. Unit coordinators provide support to their respective professional teams, allocating time for this crucial task. These teams are tasked with the development of activities focused on personal image and environmental care, with the objective of facilitating recollection of the individual's identity. |
Table 2: Main themes identified in the discourse of the reference professionals interviewed.
| Culture of care | ||
|---|---|---|
| Getting to know the person | Daily life | Bonds and relationships |
| In order to develop a comprehensive understanding of the individual's characteristics, life history, and personal preferences, the reference professional requires sufficient time. In cases of advanced dementia, it is imperative for family members and close relatives to contribute to the compilation of the individual's life story. The reference professional assumes responsibility for disseminating information to the rest of the care team regarding the individual's preferences, ensuring that daily care routines are consistently aligned with their needs and desires. | Daily routines are a critical component of the professional activities of a reference professional. The primary objective of these routines is to facilitate individuals living with dementia in performing their daily activities while ensuring consideration of their individual needs and preferences. Routines such as rising from bed, exiting from bed, eating, and participating in activities of daily life are pivotal components of a meaningful existence for these individuals. The fundamental approach entails a shift from a task-based focus to a person-centred approach. | According to reference professionals, the establishment of an emotional bond with the individual in care is of paramount importance. They emphasize the significance of relationships within the professional team and with the family. Reference professionals advocate for the involvement of families in the daily care of individuals with dementia, permitting them to enter the living unit at any time of the day. |
| Well-being | ||
| Comfort | Inclusion | Identity |
| The reference professional fulfills a fundamental need for individuals with dementia: comfort in moments of fear, loneliness, and sadness. The professional familiar with the individual has knowledge about that individual's particular concerns, worries, and history. The professional pays attention to the individual, listens to them, and offers a reassuring demeanor, which can include taking the hand of the individual and spending time to help them feel better. | The key professional is the one who recognizes the individual's need to be integrated into their family and social group. This professional enables the family's participation in the individual's daily care and fosters activities and interactions that facilitate the individual's sense of belonging to the lives of others. The key professionals interviewed underscore the positive impact of continuous contact with family and close friends on the individual's well-being. | The professional's ability to understand the individual's needs facilitates the provision of assistance in the maintenance of their sense of self. This assistance encompasses not only the cultivation of their personal image but also the selection of daily activities and the furniture and decorative elements that comprise their physical environment. The designated professional oversees the management of attire, personal care products, and other essential items, ensuring the individual's ability to preserve their identity and daily functioning. |
The unit coordinators focused their discourse on leadership and communication skills, on the creation of meaningful bonds and relationships, the flexibilization of daily routines and the carrying out of meaningful activities for people with dementia. The main themes identified are summarized in Table 1.
The reference professionals focused on the culture of care, emphasizing the importance of getting to know the person being cared for, of generating an emotional bond with them and of adapting daily routines to their preferences and desires. The identified main themes are summarized in Table 2.
Discussion
The PCC approach to dementia care entails the organization of residential facilities into living units, with each unit functioning as a domestic environment that fosters autonomy, self-expression, and personal connection. The role of direct care staff in this context is to facilitate the realization of these goals. The concept of a home as a private space, over which an individual has agency, and as the primary locus for personal relationships imbued with symbolic significance underscores the importance of maintaining living units of modest size [8].
The professionals interviewed in this study acknowledged the significance of the organizational structure of living units within the PCC approach. They emphasized the importance of fostering meaningful relationships with the individuals they support and their families, as well as among themselves as a professional team.
The discourse of the reference professionals reinforces that, under the PCC approach, the auxiliary staff does not perform daily tasks while people sit and wait; rather, the staff encourages residents to participate in the routines of the center as if it were their own home, as far as possible, and organizes the day’s routine according to their wishes and preferences. Daily life revolves around meaningful activities, such as cooking, laundry, sweeping, etc. The residents are empowered to exercise autonomy in decision-making, including the selection of meals, sleep schedules, rest, personal care routines, and activities, thereby preserving their individual lifestyles [9,10].
One of the most prevalent experiences of individuals with dementia in conventional residential facilities is a state of boredom (manifesting as monotonous days and an absence of stimulation) and a concomitant desire for enhanced social interaction. Daily activities become vehicles for social stimulation and the cultivation of satisfying relationships, while concurrently fostering individuals’ functional and cognitive abilities. The decision-making process in daily life is entrusted to the individual, rather than the organization, thereby ensuring that their wishes and desires are honored and prioritized [25]. Research has shown that music sessions, dancing, bingo, pet therapy and group storytelling are activities that have demonstrated their effectiveness in improving the well-being of both individuals with dementia and the auxiliary staff responsible for promoting and supporting the development of such activities [11,12].
In addition, professionals interviewed noted the importance of outdoor activities that are physical or social in nature, such as walking, gardening and group activities [13]. Scientific evidence shows that personalized, meaningful activities have the potential to reduce behavioral and psychological symptoms in individuals with dementia. Music, for instance, has demonstrated efficacy in reducing agitation, depression, and anxiety, while reminiscence therapies have been shown to enhance mood and cognitive functioning [14].
Unit coordinators are tasked with the responsibility of empowering direct care staff, providing autonomy in daily routines, fostering teamwork, and cultivating enriching relationships with residents [15]. The direct care staff plays a pivotal role, undertaking responsibilities that encompass food preparation, laundry, personal care, and the performance of daily activities. The emphasis is placed on routine activities and environmental details that facilitate occupational performance and quality of life. The program of activities is designed in each unit in a decentralized manner, so that activities are chosen by consensus with the people who live there. Day-to-day decisions are made by the people themselves or in conjunction with the staff, which has proven to have the potential to empower both. Most important is the sense of home, where mealtimes are an opportunity for social and community interaction [16].
Each residential center creates its own model of application of the PCC approach. However, a close examination of the discourses of the professionals interviewed reveals strong similarities with other models, such as the Green House model. In this model, nursing assistants are stably assigned to a single unit and perform a broad range of functions, including cooking, cleaning, laundry, caring for people, and facilitating activities according to the preferences of the residents. Consequently, staff members perform multiple tasks, including attending to healthcare needs, organizing activities, and household chores [17].
As indicated by the findings of multiple studies, the role of auxiliary staff in providing comfort and mitigating the fear of loneliness experienced by residents of these facilities has been identified as a crucial component in enhancing the quality of life for individuals residing in such centers. The establishment of relationships with individuals and their families is imperative to facilitate meaningful communication and support for residents in need.
The living unit becomes the person’s home and home is perceived as a place of belonging and identity, as well as the key to living a good and meaningful life. The experience of home is defined by feelings of belonging and being at home. Individuals with dementia are able to feel and appreciate living spaces. In this sense, direct care staff contribute to this purpose when they help connect people to their history, objects, activities and important life experiences [18].
In the context of direct care services, staff members who dedicate time to actively listening to individuals with dementia have been found to promote a sense of connection and enhance their well-being. However, when such opportunities for engagement are not provided, the individuals experience a sense of devaluation, which can lead to the avoidance of interactions that might jeopardize their self-esteem. Initiating a connection with the individual through verbal and nonverbal communication, eliminating anonymity by addressing the person by name and avoiding stereotypes, demonstrating respect, perceiving oneself as equal to the individual, explaining the procedures to be performed, and soliciting permission or approval are crucial components of this approach to care. Under this approach to care, professional relationships are characterized by respect and information sharing, ensuring the preservation of the individual’s personality and dignity. Conversely, staff beliefs about diminished self-worth and dignity in people with dementia can result in undignified care [19].
To ensure the provision of safe care that respects the dignity of people with dementia, staff require training to explore alternative methods for dealing with challenging situations [20-22].
In such cases, leadership and supervision are essential for providing support, guidance, and mentoring to direct care workers [23].
The interactions between direct care staff and the individuals under their care should prioritize the establishment of rapport and understanding, with a focus on attending to the wellbeing of the individuals. This approach facilitates the cultivation of a sense of safety and protection [24]. The process of familiarizing oneself with individuals living with dementia, including their preferences and life histories, enables the comprehension of their expressions, fostering a sense of familiarity, and providing reassurance during periods of disorientation. Conversations and emotional connections should be cultivated through everyday activities, particularly in intimate situations such as body care [25].
The fundamental purpose of daily activities is to support individuals in feeling that he or she is living fulfilling lives. This foundation is built on three elements: a catalytic environment, a meaningful life and a meaningful activity. The catalytic environment creates a foundation in which individuals feel safe and free to express themselves and engage in new experiences. A meaningful life entails a connection to one’s past, facilitating the maintenance of one’s identity. Additionally, meaningful activities contribute to a sense of purpose and connection to the present. In this regard, the role of direct care staff is paramount, as they facilitate the exploration of emotions and diversity within the environment, thereby enhancing fulfillment [26,27].
In person-centered care, the quality of care is contingent on the empathy of caregivers and their ability to facilitate activities that are congruent with the life history, preferences, and abilities of the individual [28]. The leadership role of direct care staff is also imperative, necessitating training to develop personalized care plans that encompass the life history, preferences, and needs of each individual [29].
The discourse of the professionals interviewed highlights the need for training in addressing behaviors such as wandering, agitation and social isolation in individuals with dementia under the Person-Centered Care (PCC) approach [30-32]. In this regard, it is important that coordinators use transformative leadership techniques by being present in the units on a daily basis and demonstrating how to perform tasks. In this way, nursing assistants can feel supported and committed to care [33].
Conclusion
In the context of Person-Centered Care (PCC) with dementia, a personalized care approach is adopted that recognizes the uniqueness of each individual and facilitating the comprehension of the world from the perspective of the care staff. In residential centers where people with dementia live, the application of this approach necessitates the organization of care in living units comprising a limited number of individuals and the establishment of unit coordinator and reference professional roles. These professionals adopt a transformational leadership style that enables them to translate their clear and coherent vision of PCC into daily practice. They form cohesive professional teams that promote people’s well-being, autonomy and independence, while reinforcing their identity, sense of control over their environment and sense of home.
This approach has an important basis on the ethics of care and values that professional practice must reflect to become normative. To exemplify this leadership style, leaders must be present in the units where people reside and where auxiliary personnel carry out their activities. This presence enables leaders to assess their skills and select the most appropriate leadership behavior in each situation: direction, coaching, support, or delegation.
Author declarations
Declaration of interest: The authors declare no conflicts of interest or financial disclosures related to this research.
References
- Kitwood T. The experience of dementia: Improving care. Relat Exp Stories Heal Soc Care. 2004; 1: 106-10.
- Catela-Huertas A, Pinzón-Pulido S, Fuentes-Maltés PJ, Fernández Portero C. Keys to the well-being of people with dementia living in residential facilities. Meta-review and metasynthesis. Psicogeriatría. 2024; 14: 57-70.
- Shier V, Khodyakov D, Cohen LW, Zimmerman S, Saliba D. What does the evidence really say about culture change in nursing homes? Gerontologist. 2014; 54: 6-16.
- Rojano i Luque X, Serra Marsal E, Soler Cors O, Salvà Casanovas A. Impact of person-centered care (PCA) on quality of life, well-being and coping. A cross-sectional study. Rev Esp Geriatr Gerontol. 2021; 56: 29-34.
- Brooker, D. What is person-centred care in dementia? Reviews in Clinical Gerontology. 2004; 13: 215-222.
- Martínez T, Suárez-Álvarez J, Yanguas J. Impact in residences of person-centered care (PCA) on quality of life, well-being and coping. Cross-sectional study. Spanish Journal of Geriatrics and Gerontology. 2020; 55: 208-214.
- Diaz-Veiga P, Sancho-Castiello M, Martínez-Rodríguez T. [Living units for the elderly in the framework of the deinstitutionalization process]. Zerbitzuan. 2022; 78: 51-66.
- Fleming A, Kydd A, Stewart S. Care homes: The developing ideology of a homelike place to live. Maturitas. 2017; 99: 92-97
- Verbeek H, Van Rossum E, Zwakhalen SMG, Kempen GIJM, Hamers JPH. Small, homelike care environments for older people with dementia: A literature review. Int Psychogeriatrics. 2009; 21: 252-264.
- Tierney L, Beattie E. Enjoyable, engaging and individualised: A concept analysis of meaningful activity for older adults with dementia. Int J Older People Nurs. 2020; 15: 1-13.
- Shiells K, Holmerova I, Stefl M, Stepankova O. Electronic patient records as a tool to facilitate care provision in nursing homes: An integrative review. Inform Health Soc Care. 2019; 44: 262-77.
- Sion KYJ, Verbeek H, Zwakhalen SMG, Odekerken-Schroder G, Schols JMGA, Hamers JPH. Themes Related to Experienced Quality of Care in Nursing Homes From the Resident’s Perspective: A Systematic Literature Review and Thematic Synthesis. Gerontol Geriatr Med. 2020; 6.
- Chaudhury H, Hung L, Badger M. The role of physical environment in supporting person-centered dining in long-term care: A review of the literature. Am J Alzheimers Dis Other Demen. 2013; 28: 491-500.
- Travers C, Brooks D, Hines S, O’Reilly M, McMaster M, He W, et al. Effectiveness of meaningful occupation interventions for people living with dementia in residential aged care: a systematic review. JBI database Syst Rev Implement reports. 2016; 14: 163-225.
- Brownie S, Nancarrow S. Effects of person-centered care on residents and staff in aged-care facilities: A systematic review. Clin Interv Aging. 2013; 8: 1-10.
- Bortnick KN. An Ecological Framework to Support Small-Scale Shared Housing for Persons with Neurocognitive Disorders of the Alzheimer’s and Related Types: A Literature Review. Hong Kong J Occup Ther HKJOT. 2017; 29: 26-38.
- Ausserhofer D, Deschodt M, De Geest S, van Achterberg T, Meyer G, Verbeek H, et al. “There’s No Place Like Home”: A Scoping Review on the Impact of Homelike Residential Care Models on Resident-, Family-, and Staff-Related Outcomes. J Am Med Dir Assoc. 2016; 17: 685-693.
- Førsund LH, Grov EK, Helvik A-S, Juvet LK, Skovdahl K, Eriksen S. The experience of lived space in persons with dementia: a systematic meta-synthesis. BMC Geriatr. 2018; 18: 33.
- Torossian MR. The dignity of older individuals with Alzheimer’s disease and related dementias: A scoping review. Dementia. 2021; 20: 2891–2915.
- Cleland J, Hutchinson C, Khadka J, Milte R, Ratcliffe J. What defines quality of care for older people in aged care? A comprehensive literature review. Geriatr Gerontol Int. 2021; 21: 765-778.
- Mohr W, Rädke A, Afi A, Edvardsson D, Mühlichen F, Platen M, et al. Key intervention categories to provide person-centered dementia care: A systematic review of person-centered interventions. J Alzheimer’s Dis. 2021; 84: 343-366.
- O’Donnell E, Holland C, Swarbrick C. Strategies used by care home staff to manage behaviour that challenges in dementia: A systematic review of qualitative studies. Int J Nurs Stud. 2022; 133: 104260.
- Morgan DG, Stewart NJ, D’Arcy C, Cammer AL. Creating and sustaining dementia special care units in rural nursing homes: the critical role of nursing leadership. Nurs Leadersh (Tor Ont). 2005; 18: 74-99.
- Wu Q, Qian S, Deng C, Yu P. Understanding Interactions Between Caregivers and Care Recipients in Person-Centered Dementia Care: A Rapid Review. Clin Interv Aging. 2020; 15: 1637-1647.
- Adlbrecht L, Bartholomeyczik S, Hildebrandt C, Mayer H. Social interactions of persons with dementia living in special care units in long-term care: A mixed-methods systematic review. Dementia. 2021; 20: 967-984.
- Strick K, Abbott R, Coon JT, Garside R. Meta-ethnography of the purpose of meaningful occupation for people living with dementia. Int J Older People Nurs. 2021; 16: 1-17.
- Groenendaal M, Smaling HJA, Achterberg WP, Caljouw MAA. Maintaining meaningful activities for persons with dementia during transitions of care: A systematic review. Geriatr Nurs. 2022; 44: 176-183.
- Li J, Porock D. Resident outcomes of person-centered care in long-term care: A narrative review of interventional research. Int J Nurs Stud. 2014; 51: 1395-1415.
- Kim SK, Park M. Effectiveness of person-centered care on people with dementia: a systematic review and meta-analysis. Clin Interv Aging. 2017; 12: 381-397.
- Piirainen P, Pesonen HN, Kyngäs H, Elo S. Challenging situations and competence of nursing staff in nursing homes for older people with dementia. Int J Older People Nurs. 2021; 00: e12384.
- Leung JLM, Sezto NW, Chan WC, Cheng SP, Tang SH. Attitudes and perceived competence of residential care homes staff about dementia care. Asian J. Gerontol. Geriatr. 2013; 8: 21-29.
- Boumans J, van Boekel L, Kools N, Scheffelaar A, Baan C, Luijkx K. How staff characteristics influence residential care facility staff’s attitude toward person-centered care and informal care. BMC Nurs. 2021; 20: 217.
- Rokstad AM, Vatne S, Engedal K, Selbæk G. The role of leadership in the implementation of person-centred care using Dementia Care Mapping: a study in three nursing homes. J Nurs Manag. 2015; 23: 15-26.